This is a common scenario and one you will certainly be asked about in exams and in the trauma meeting.
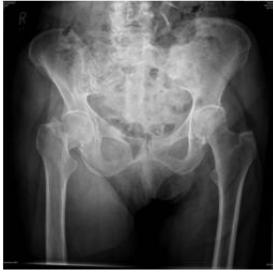
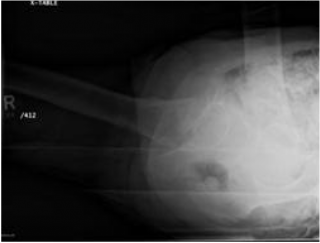
A 92 year old lady fell when the driver of a bus braked too hard. She was unable to mobilize due to right hip pain. She is otherwise healthy and mobilizes normally with one stick. Her leg is short and externally rotated. Her radiographs are shown below.
A 92 year old lady fell when the driver of a bus braked too hard. She was unable to mobilize due to right hip pain. She is otherwise healthy and mobilizes normally with one stick. Her leg is short and externally rotated. Her radiographs are shown below.
What are your management priorities?
How would you definitively treat this (fixation with screws, hemi-arthroplasty, total hip replacement, dynamic hip screw) and what are the controversies?
Are there any guidelines that would help?
This lady has a displaced intracapsular left neck of femur fracture. She should be resuscitated and then admitted promptly. She should be assessed routinely by the orthogeriatricians and operated on within 36 hours (BOA standard for trauma). NICE guidelines suggest the femoral head should be replaced (hemi or THR) and in this case a total hip replacement could be argued (she walks with only one stick, is not cognitively impaired and is medically fit) . An anterolateral approach and cemented components are preferable.
BOAST guidelines:
How would you definitively treat this (fixation with screws, hemi-arthroplasty, total hip replacement, dynamic hip screw) and what are the controversies?
Are there any guidelines that would help?
This lady has a displaced intracapsular left neck of femur fracture. She should be resuscitated and then admitted promptly. She should be assessed routinely by the orthogeriatricians and operated on within 36 hours (BOA standard for trauma). NICE guidelines suggest the femoral head should be replaced (hemi or THR) and in this case a total hip replacement could be argued (she walks with only one stick, is not cognitively impaired and is medically fit) . An anterolateral approach and cemented components are preferable.
BOAST guidelines:
- Prompt admission (<4 hours) to ward
- Secondary prevention and falls assessment
- Multidisciplinary team management
- MRI if X-rays are inconclusive
- Immediate and sufficient analgesia
- Identify and treat co-morbidities so as not to delay surgery
- Operate within 36 hours on a planned trauma list
- Operate to allow the patient to fully weight bear
- Orthogeriatric input and assessment within 72 hours
- Assess for cognitive impairment and delirium
- Consider surgery even if it is palliative
- DVT prophylaxis
- Educate patient and family about treatment, care and rehabilitation
- Submit data to National Hip Fracture database
 RSS Feed
RSS Feed
