Assessment and management of lower limb long bone fractures
by James Donaldson
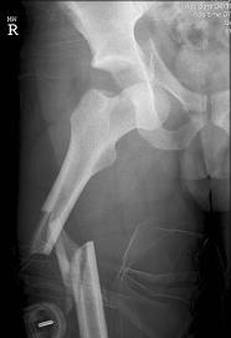
Femur shaft fracture
|
History:
Age – young, high energy energy, often associated with life-threatening trauma. In elderly due to osteoporosis and low energy fall Occupation. Mechanism of injury - often road traffic collision Time/date of injury Past medical/surgical history Medication/drugs and allergies Last ate/drank (for timing of emergency surgery if needed) Radiographs / Imaging:
|
Symptoms and signs:
- Pain, swelling and deformity in the thigh
- Unable to weight bear
- Ipsilateral femoral neck # seen in 2-6% but missed in up to 30% of cases
- Document neurovascular status
Initial management:
- ATLS principles. This is a significant injury
- Analgesia, IV fluids, skin traction for comfort
- Assess for other injuries
- Admit for surgical fixation. In elderly liaise with care of the elderly team if appropriate
- Call senior if patient is unstable, polytrauma, open fracture or neurovascular compromise
Definitive treatment:
- Nearly all need operative fixation
- Intramedullary femoral nail - Antegrade is gold standard
- Consider damage control if polytrauma patient, neurovascular injury or significant soft tissue compromise
Complications:
- Malunion: sagittal, coronal, rotational, length
- Delayed union
- Nonunion
- Heterotopic ossification
- Infection
- Iatrogenic #
- Neurovascular injury
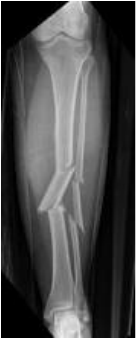
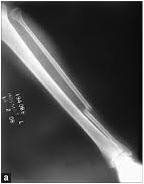
Tibial shaft fracture
Symptoms and signs:
- Compartments – commonest location of compartment syndrome
- Neurovascular status
- Associated injuries
- Commonest long bone #
- Pain, swelling, deformity, inability to weight bear
- Crucial to assess:
- Compartments – commonest location of compartment syndrome
- Neurovascular status
- Associated injuries
Open fracture classification (Gustillo and Anderson) of open fractures:
Grade - 1. Wound <1cm. Often inside out injury
2. Wound 1-10cm. Mild – moderate periosteal stripping
3. a) significant soft tissue injury but adequate periosteal coverage
b) as above but inadequate periosteal and soft tissue coverage. Will require a flap
c) associated vascular injury requiring repair
Grade - 1. Wound <1cm. Often inside out injury
2. Wound 1-10cm. Mild – moderate periosteal stripping
3. a) significant soft tissue injury but adequate periosteal coverage
b) as above but inadequate periosteal and soft tissue coverage. Will require a flap
c) associated vascular injury requiring repair
Initial management:
- Photograph and dress the wound
- Antibiotics (1.2g co-amoxiclav or 600mg clindamycin if allergic) and anti-tetanus
- Limb splintage eg. above knee backslab
- Compartment syndrome
- Devascularised limb
- Multiply injured patient
- ATLS principles. This is a significant injury
- Analgesia, IV fluids, skin traction for comfort
- Admit for surgery. Call senior if open, neurovascular compromise or polytrauma
- Open fracture management (see BAPRAS guidelines):
- Photograph and dress the wound
- Antibiotics (1.2g co-amoxiclav or 600mg clindamycin if allergic) and anti-tetanus
- Limb splintage eg. above knee backslab
- Immediate debridement if:
- Compartment syndrome
- Devascularised limb
- Multiply injured patient
- Otherwise debridement <24hrs of injury
Definitive treatment:
- Early debridement with further co-amoxiclav and 1.5mg/kg gentamicin
- Continue co-amoxiclav for until soft tissue closure or maximum of 72hrs
- At the time of stabilization vancomycin 1g or teicoplanin 800mg should be given
- Spanning ex-fix if the fracture is not definitively stabilized or the skin not closed at primary debridement
- Convert to definitive internal stabilization as early as possible if soft tissues allow – usually intramedullary nail
Complications:
- Malunion: sagittal, coronal, rotational, length
- Delayed union
- Nonunion
- Knee pain (if IM nail in >50%)
- Infection
- Compartment syndrome (1-9%)
- Neurovascular injury
Consider primary amputation if:
- Uncontrollable haemorrhage
- Incomplete traumatic amputation
- Segmental muscle loss > 2compartments
- Bone loss > 1/3 of tibia
- Avascular >6hrs
- 2 consultant decision
Fibula shaft fractures
|
Isolated shaft fracture:
Associated with tibial shaft fracture:
Maisonneuve fracture:
|