Assessment and management of proximal femur fractures
by James Donaldson
Scenario: called to A&E to assess a 89 year old lady with low energy fall and shortened externally rotated leg.
History:
Age
Time/date of injury
Past medical/surgical history
Fitness for anaesthesia
Co-morbidity
Anticoagulation
Medication/drugs and allergies
Social history
Where do they live? House/flat/bungalow, nursing home
Social support, mobility aids, home help, carer, family involvement
AP pelvis and lateral hip X-rays
If the diagnosis is in doubt MRI (CT if not available) should be performed as soon as possible.
History:
Age
Time/date of injury
Past medical/surgical history
Fitness for anaesthesia
Co-morbidity
Anticoagulation
Medication/drugs and allergies
Social history
Where do they live? House/flat/bungalow, nursing home
Social support, mobility aids, home help, carer, family involvement
AP pelvis and lateral hip X-rays
If the diagnosis is in doubt MRI (CT if not available) should be performed as soon as possible.
|
Injury
features
Low energy injury in elderly Consider stress fracture in young patient with unaccustomed or repetitive strenuous activity High energy trauma in young Secondary to metastatic disease |
Signs and Symptoms
Short, externally rotated leg following innocuous fall Unable to walk Recent change in activity Insidious onset Relief of pain with rest Associated with multiple injuries. ATLS protocol History of cancer (breast, lung, thyroid, kidney, prostate commonly) |
X-rays & Management
|
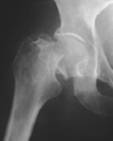
Intra-capsular fracture
|
Management
|
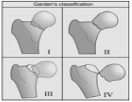
Classification and Treatment
|
|
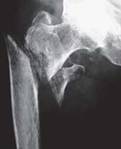
Extra-capsular fracture
|
Management
Principles as above except for the urgent need for fixation – capsular blood supply is not compromised |
Treatment
|
British Orthopaedic Association Standards of Care for patients with fragility hip fractures:
- Prompt admission (<4 hours) to ward
- Secondary prevention and falls assessment
- Multidisciplinary team management
- MRI if X-rays are inconclusive
- Immediate and sufficient analgesia
- Identify and treat co-morbidities so as not to delay surgery
- Operate within 36 hours on a planned trauma list
- Operate to allow the patient to fully weight bear
- Orthogeriatric input and assessment within 72 hours
- Assess for cognitive impairment and delirium
- Consider surgery even if it is palliative
- DVT prophylaxis
- Educate patient and family about treatment, care and rehabilitation
- Submit data to National Hip Fracture database